EMH Schweizerischer Ärzteverlag AG
Farnsburgerstrasse 8
CH-4132 Muttenz
+41 (0)61 467 85 44
support@swisshealthweb.ch
www.swisshealthweb.ch
Published on 01.09.2022
The impact of a structured institutional lead management programme on TLE outcomes is investigated.
| Diagnostic procedure | Main focus | When to perform |
| Medical history | CIED implantation indication, drugs, allergies, other comorbidities. | Always before intervention |
| Analysis of implantation reports | Implanted material, vascular access routes, challenges during implantation. | Always before intervention |
| CIED interrogation | Analysis of CIED function and PM dependency. In case of lead malfunction provocation maneuvers and EGM evaluation. | Always before intervention |
| Transthoracic echocardiography | Biventricular function, lead vegetations, presence of concomitant significant valve disease (vegetations, tricuspid regurgitation), pre-operative risk stratification. | Always before intervention |
| Transoesophageal echocardiography | Lead insertion points, vegetations, pericardial and pleural effusions, presence of right-to-left shunt, hemodynamics. | (Before and) during intermediate and high-risk TLE |
| Fluoroscopy and subclavian venography | Lead defects, patency of access routes, assessment of connective tissue bridges and lead insertion points, vessel stenosis. | Mostly before intervention |
| Laboratory tests | Electrolytes, creatinine, coagulation, blood count and group for potential transfusion. | Immediately before intervention |
| FDG-PET scan | Evidence for CIED infection. | In case of discrete signs of (pocket) infection |
| Thoracic CT/MRI | General anatomy, lead insertion site, vascular access/occlusion. | In complex situations or perforated leads |
| Coronary angiography and cardiac catheterisation | Presence of significant concomitant coronary artery disease, grading of valve disease. | In case of planned hybrid procedure involving surgery |
| Individualised cumulative risk assessment | Calculation of interventional risk for interdisciplinary decision on optimal lead management strategy. | Always before definite intervention planning |
| Patient characteristics | 2013–2018 (n = 84) | 2019–2020 ( n=92 ) | p-value |
| Clinical characteristics | |||
| Female sex | 27 (32%) | 29 (32%) | 1 |
| Age (years) | 69 (54–76) | 69 (54–75) | 0.58 |
| Body height (m) | 1.71 (1.65–1.76) | 1.72 (1.65–1.78) | 0.35 |
| Body weight (kg) | 75 (65–90) | 80 (69–90) | 0.12 |
| LVEF (%) | 55 (35–65) | 57 (36–61) | 0.76 |
| Arterial hypertension | 53 (64%) | 58 (63%) | 1 |
| Diabetes | 20 (24%) | 18 (20%) | 0.62 |
| Renal failure | 22 (27%) | 23 (26%) | 0.95 |
| Pacemaker dependency | 38 (45%) | 53 (58%) | 0.14 |
| Prior cardiac surgery | 27 (33%) | 22 (24%) | 0.27 |
| Drug therapy | |||
| Oral anticoagulation | 42 (50%) | 47 (52%) | 1 |
| Antiplatelet therapy | 43 (51%) | 24 (26%) | <0.001 |
| Betablocker | 52 (62%) | 53 (58%) | 0.67 |
| ACE inhibitor or AT2 blocker | 42 (51%) | 58 (63%) | 0.11 |
| CIED system | |||
| Single- or dual-chamber PM | 45 (54%) | 50 (54%) | 1 |
| CRT-P | 3 (4%) | 3 (3%) | 1 |
| Single- or dual-chamber ICD | 25 (30%) | 22 (24%) | 0.48 |
| CRT-D | 11 (13%) | 17 (18%) | 0.44 |
| CIED indication | |||
| Sinus node disease | 13 (15%) | 16 (17%) | 0.89 |
| AV block | 29 (35%) | 31 (34%) | 1 |
| Ventricular tachycardia/fibrillation | 13 (15%) | 18 (20%) | 0.61 |
| Other | 29 (35%) | 27 (29%) | 0.57 |
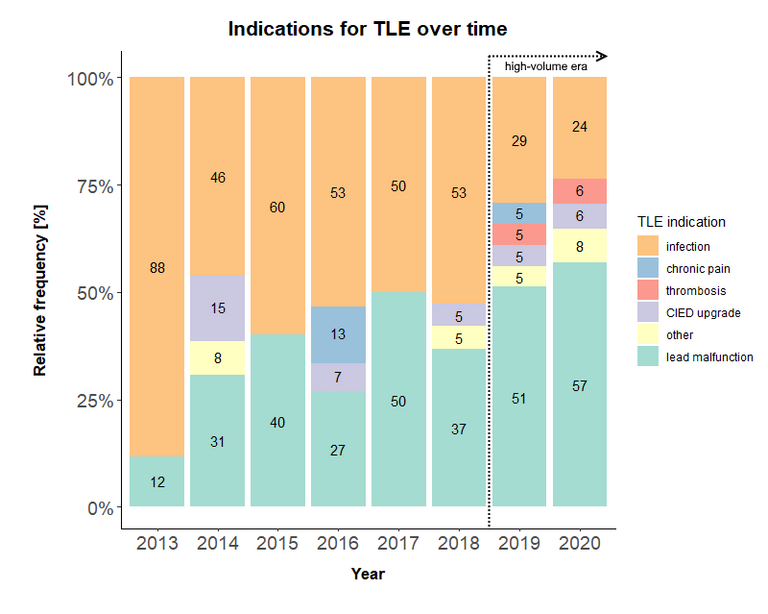
| TLE indication | |||
| CIED or systemic infection | 50 (60%) | 24 (26%) | <0.001 |
| Non-infectious indication | 34 (40%) | 68 (74%) | <0.001 |
| – Lead malfunction | 26 (31%) | 50 (54%) | 0.003 |
| – Chronic pain | 2 (2%) | 2 (2%) | 1 |
| – Thrombosis / venous occlusion | 0 (0%) | 5 (5%) | 0.06 |
| – Device upgrade | 4 (5%) | 5 (5%) | 1 |
| – Other | 2 (2%) | 6 (7%) | 0.28 |
| Procedural characteristics | 2013–2018 (n = 84) | 2019–2020 (n = 92) | p-value |
| Procedural setting | |||
| Emergency procedure | 21 (25%) | 15 (16%) | 0.21 |
| Intervention site | 0.003 | ||
| – Electrophysiology laboratory | 19 (23%) | 6 (7%) | 0.005 |
| – Hybrid operation room | 64 (76%) | 85 (92%) | 0.006 |
| – Conventional operation room | 1 (1%) | 1 (1%) | 1 |
| Procedural details | |||
| Procedure duration (min) | 144 (110–196) | 143 (85–240) | 0.93 |
| Passive leads | 34 (25%) | 23 (15%) | 0.06 |
| Number of targeted leads for extraction | 2 (1–2) | 2 (1–2) | 0.40 |
| Lead dwell time (years) | 4.3 (1.8–8.6) | 4.4 (2.4–8.4) | 0.43 |
| Use of conventional stylets | 18 (22%) | 21 (23%) | 0.43 |
| Use of locking stylets | 65 (78%) | 71 (77%) | 0.97 |
| Use of laser sheath | 22 (27%) | 0 (0%) | <0.001 |
| Use of mechanical non-powered sheath | 45 (70%) | 35 (39%) | <0.001 |
| Use of rotational mechanical sheath | 2 (3%) | 34 (38%) | <0.001 |
| Use of femoral snares | 4 (5%) | 12 (13%) | 0.10 |
| Procedural outcomes | |||
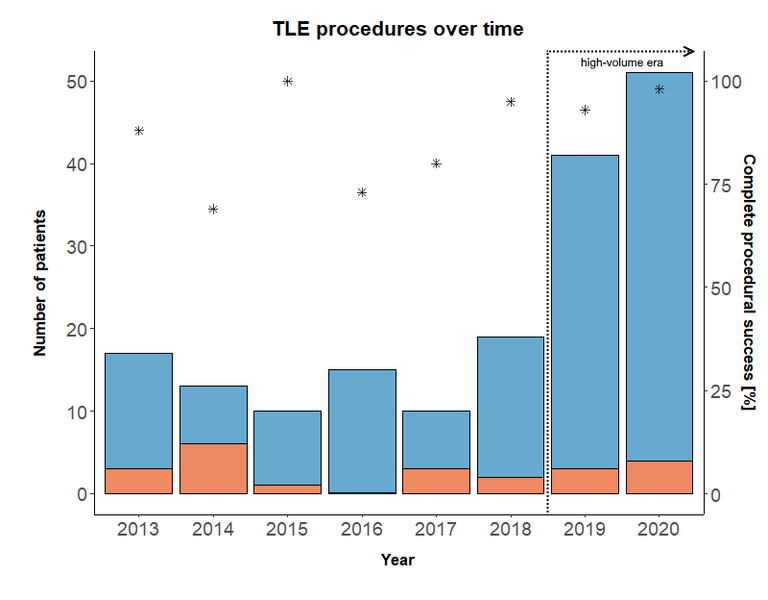
| Clinical success | 76 (90%) | 90 (98%) | 0.020 |
| Complete procedural success | 71 (85%) | 87 (95%) | 0.027 |
| Duration of hospital stay (days) | 6 (4–13) | 3 (3–6) | <0.001 |
| Total complications | 15 (18%) | 7 (8%) | 0.07 |
| Major complications | 4 (5%) | 0 (0%) | 0.05 |
| – Procedure related deaths due to vessel laceration, haemothorax | 2 (2%) | 0 (0%) | 0.23 |
| – Cardiac tamponade requiring surgery | 1 (1%) | 0 (0%) | 0.47 |
| – Thromboembolic event requiring surgery | 1 (1%) | 0 (0%) | 0.471 |
| – Stroke | 0 (0%) | 0 (0%) | – |
| Minor complications | 11 (13%) | 7 (8%) | 0.34 |
| – Femoral bleeding | 0 (0%) | 2 (2%) | 0.50 |
| – Pocket haematoma | 5 (6%) | 0 (0%) | 0.023 |
| – Other | 6 (7%) | 5 (5%) | 0.76 |
Published under the copyright license.
"Attribution - Non-Commercial - NoDerivatives 4.0"
No commercial reuse without permission.
See: emh.ch/en/emh/rights-and-licences/